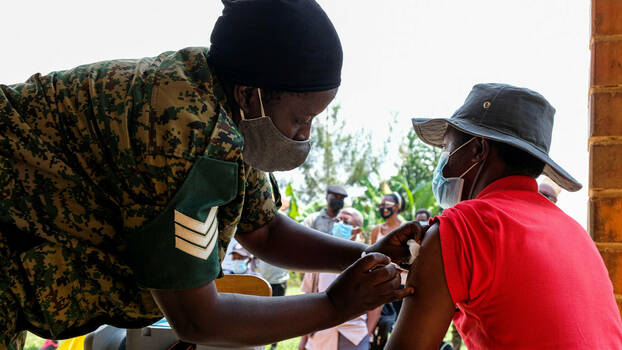
On 18 June 2021, the Ugandan government re-instituted a 42-day lockdown following an intense surge in COVID-19 infections. A Ugandan Ministry of Health report in the days leading up to the lockdown had indicated that the intensity and severity of the illness had grown exponentially compared to the first wave, with the most affected age group being 20–39-year-olds. The report also noted that while it took three to four months for the first wave to become a pandemic, it had taken less than ten days for the second. The new wave was attributed to the more transmittable Delta variant, while, according to the World Health Organization, new weekly cases across Africa have now exceeded half of the second-wave peak of more than 224,000 in early January.
Samuel Kasirye works as a Programme Manager at the Rosa Luxemburg Foundation’s East Africa Office in Dar es Salaam, Tanzania.
The response to the second wave in Uganda has been messy, worsened by the lack of a robust health care system, an acute vaccine shortage, and let-downs in managing the wider ramifications of the lockdown, especially for economically vulnerable populations. The current strategies to address the COVID–19 pandemic by the government led by General Yoweri Museveni have provoked some of the most polarized debates in the country, with many politicians and medical experts accusing him of ineptness in managing the crisis. Stories of hospitals facing difficulties in securing bottled oxygen, lack of adequate Personal Protective Equipment, inadequate intensive care units, and militarization of the health care disaster have been widely reported.
To add to this convolution, regional and continental efforts to contain the virus have suffered setbacks due to the complexity of the international vaccine access regime. According to a recent article in The East African, the African Union expressed concerns about the European Union’s apparent discriminatory policy in enacting travel bans for people vaccinated with the WHO-backed AstraZeneca vaccine produced in India. The AU also cited bias in the global distribution system, which has made few doses available to Africa (largely delivered through donations from wealthy countries), thereby making it almost impossible to quicken the commercial vaccine rollout across the continent.
Beyond this absurdity, however, the lack of transparency and accountability within individual African countries is adding further complexity that aggravates a worsening public health and economic situation. In Uganda, these internal failures have resulted in widespread public anger and collapsing public trust, which is a key component to fighting the pandemic. One-and-a-half years into the COVID-19 crisis, the government’s promised interventions have not materialized, despite heavy borrowing and large grants from “development” partners. The borrowing, which has surged especially since the crisis started, is starting to become a serious concern now that is has risen to 50 percent of GDP.
Ballooning Debt, Spiralling Crisis
Ugandan finance minister Matia Kasaija, who previously argued that the nation’s debt was still within sustainable limits, recently conceded that it had reached worrying levels, especially after the government obtained another 1 billion US dollars from the IMF in the form of a COVID-19-related loan. The loan in question seeks to support short-term responses to the COVID-19 crisis and sustain a post-crisis recovery through a number of reforms focused on creating fiscal space for priority social spending, preserving debt sustainability, strengthening governance, and enhancing the country’s monetary and financial sector framework.
However, the lack of proper accountability and the seemingly haphazard management of COVID-19-related resources has spurred a number of key demands from the population. The leader of the opposition in parliament, the Hon. Mathias Mpuuga, has accused the government of misusing the first tranche of loans and grants disbursed during the first outbreak last year. His argument was supported by Uganda’s Auditor General, who cited non-compliance with procurement laws, unaccounted funds, diversions, inadequate valuation of in-kind donations, and poor management of quarantine centres.
Members of Parliament are also questioning funds allocated to the security sector, which has been the recipient of frequent supplementary budgets, most of which are classified—thereby enabling them to escape public scrutiny. Hon. Kasaija argues differently and notes that addressing a pandemic in a country such as Uganda is highly complex, given the need to balance economic, social, and health priorities. Since March 2020, he contends, domestic containment measures have caused economic and social strife, particularly affecting agriculture, industry, and the service sector, all of which are vital to the Ugandan economy.
Therefore, it is not surprising that the second wave of COVID-19 has raised deep questions on a number of fronts, including the government’s commitment to managing the health crisis and responding to basic emergencies during the lockdown. For instance, it has taken the government more than three weeks to distribute the first tranche of cash assistance to the 500,000 most economically vulnerable families. Dr. Kiiza Besigye, one of General Museveni’s most vocal critics, has been insisting since March of last year that the government establish a legal and institutional framework for managing COVID-19, reasoning that the pandemic cannot be handled by politicians and the military alone. COVID-19 has largely been managed through the Office of the Prime Minister and Resident District Commissioners (RDCs) instead of senior medical officers within the Ministry of Health.
The Role of the State
The deficiencies in the government’s response have allowed private health care providers to exploit a fragile public health system, charging patients exorbitant fees with unusual requirements for patients to cash deposits before admission. Currently, a COVID-19 patient in a privately run facility requiring an ICU bed pays a minimum of 600 US dollars daily, which is over five times the average monthly income in the country.
A representative from the Uganda National Association of Private Hospitals (UNAPH) told a parliamentary committee debating matters relating to COVID-19 management that Uganda was a “free market” and that its members were only responding to supply and demand. The association says that the proprietors of private hospitals are filling the health care gaps worsened by years of inattention and government underfunding. The association maintains that the private hospitals were simply providing what COVID-19 patients desperately need.
These new realities have revived the debate around the state’s role in development. Dr. Ramathan Goobi, a board member of the reconstituted Uganda Development Corporation, argues that discussions about the role of the state have been ideologically discredited for over three decades. He adds that for a long time, African governments have had a flawed interpretation of the state’s role, leading to the gradual dismantling of these countries. The current challenges demonstrate that African states should adopt broader development goals, while also addressing the coordination failures that have emerged during the pandemic. Most importantly, they must build up a robust accountability system.
On a more optimistic note, last week the High Court in Kampala issued orders compelling the government to regulate the skyrocketing medical fees currently charged for treating COVID-19 patients. This followed a consent agreement between government representatives and health rights organizations under the leadership of the Centre for Human Rights and Development, which had petitioned the court. The suit elaborated that the Uganda Medical and Dental Practitioners Council and the Ministry of Health had failed to rein in private health care providers. The petitioners argued that the Ministry of Health neglected its duty to regulate fees charged by private hospitals and clinics under the Public Health Act and the Medical and Dental Practitioners Act. The petitioners had asked the court to force the Ministry of Health to extend its mandate beyond regulating health care investment in the private sector, and to ensure that quality and affordable services are delivered to patients.
The national, regional, and even global debates sparked by the COVID-19 pandemic and government interventions are likely to raise deeper questions of governance in Africa. Key questions revolve around how long the pandemic will last, what scenarios are likely should new variants continue to emerge, and how the continent will muscle the resources to fund its own vaccines and treatment. Another key question is around the “easy” access to IMF and World Bank loans and their long-term implications for countries like Uganda. Countries need to question the concealed interests behind these emerging trends. Civil society must continuously demand transparency and accountability from both governments and multilateral lenders.
What is critical for Uganda at this time is an inclusive recovery strategy centred on redistributing productive assets more equitably, with national and regional interventions reaching where they are most needed. Depending on which direction the country takes, these conversations are critical for determining Uganda’s resilience and how the state effectively responds to the crisis at hand.